The modern woman is task-oriented. She lives in a world demanding of her competence, attention, and efficiency. We use technology, tap into our communities, plumb the depths of our reserves to navigate an often hyper-masculinized world while retaining our most vital feminine powers. The power that fundamentally defines our exemption from this contemporary lifestyle trajectory is baby making.
This primal empowerment forms the bedrock of a woman’s most untouchable gifts.
We have lost sight of this fact; however, and have allowed our inner compass to be co-opted. It’s certainly no wonder, that after 9 months of hypermedicalized pregnancy “management” (often following months to years of assisted reproductive technologies), birth is considered another task on the to-do list to complete.
As a type-A taskmaster, myself, I understand the lure of a predictable and painless depositing of your newborn after the long and fear-punctuated journey of pregnancy.
I’m here to tell you; however, what your obstetrician won’t.
Labor is a physiologic process that recruits neurochemical, endocrine, and immune systems into a dance that we barely have the tools to conceptualize.
When we meddle with this, when we attempt to standardize it, we put women and their babies at grave risk – physically, psychologically, and even spiritually. We rob women of an opportunity for psychospiritual transcendence.
As a science-minded medical doctor, I don’t wield this phrase with ease!
The process of conception, gestation, and birth cannot, however, be reduced to daily activities and routine life occurrences. There is something built into our consciousness that makes room for its own expansion around these life transitions. The process of bodily separation – woman from her newborn – involves a passage through a space of trance-like awareness.
I can only describe it as the sensation of floating and grounding, simultaneously. It is an experience that demands we move out of the space of our mind and into a space of sensation without judgment. It is being present, truly present, to behold a glimpse of what we are capable of as mammals and most importantly, as a human female.
In this way, a natural birth is an opportunity for redefinition and reconnection to one’s most core self. It is the way women were intended to pass through the gates of motherhood, to the next chapter of their actualization.
If you buy the potential significance of these considerations, you may want to know what represents your greatest obstacle and impediment in achieving this life milestone. You may be surprised to learn that it is epidural anesthesia. This discussion is meant to shine a light on elective epidurals – that, “Why not? Who wants to feel crazy intense pain?” choice that 2/3rds of women (and up to 90% in some hospitals) opt for every day. In my opinion, the epidural intervention is the most reprehensible of all – because of its largely dismissed risk profile, and because of its auspicious position in a cascade of interventions, unnecessary, ill-conceived, and rife with unintended consequences including death.
If we can empower women to question the validity of this procedure, then they can retain the right to preserve the integrity of their birth experience.
What’s the big deal with Epidurals?
A 60% rise in C-sections since 1996 is prompting the American College of Obstetricians and Gynecologists to fidget self-consciously in their white coats. A study revealing the prolongation of the second stage of labor thanks to epidurals has been influential in identifying the iatrogenesis – doctor-caused harm – at the root of the cesarean problem.
It appears that, thanks to an antiquated but still sanctioned construct – Friedman’s curve – the hospital clock starts ticking loudly upon arrival, and the alarm goes off after 3 hours of second stage labor with an epidural. At this non-evidence-based juncture, interventions including IV fluids, continuous monitoring, food and drink restriction, and immobilization conspire to invite pitocin, forceps, episiotomy, and surgery into the delivery room.
Obstetrics is vulnerable to practicing consensus medicine – habitual practice that is not predicated on sounds science. As I discuss here, metanalysis has demonstrated that only 30% of current obstetrical recommendations are based on quality data. What’s the rest based on? Fear-mongering and personal opinion? Let’s look at what the evidence suggests about the risks of epidurals, considering that up to 41% of women never properly consented for this intervention.
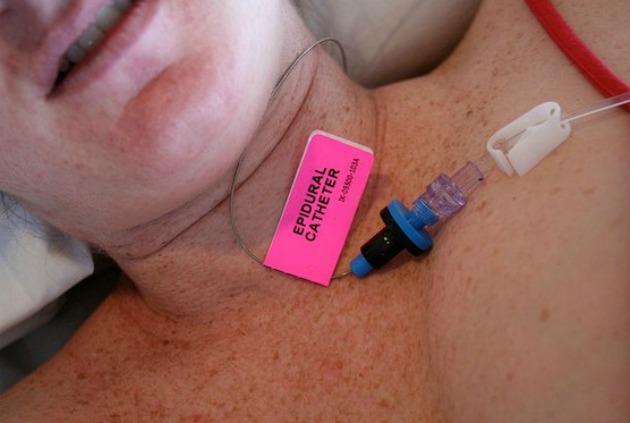
Epidurals are offered with a plethora of accoutrements including catheters for involuntary urination, blood pressure monitoring and IV fluids for changes to vascular physiology, and continuous fetal monitoring because of risk to the baby of decreased oxygen flow.12
The changes to natural labor progression are compounded by risk of fever in the mother that leads to further separation of mom and baby after birth, secondary to testing and assessment for infection. This separation represents a stress to the shared adaptation to early postpartum life and may predispose to psychiatric pathology in both mom and baby through early epigenetic influences on gene expression.345
This separation may also interfere with breastfeeding establishment. In this way, epidurals may be directly and indirectly responsible for breastfeeding struggles67. Breastfeeding appears to prevent the onset of postpartum depression if it is established within 3 months, in addition to being a continual source of immunologically essential information trafficked from mom to baby.
Shooting Up You and Your Baby
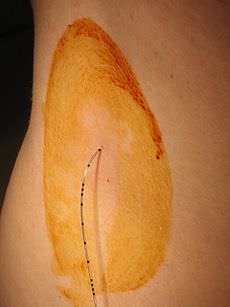 Epidurals are a delivery method for narcotic pain-killers that pass through the placenta to the baby and have largely unpredictable effects on the birthing woman. Evidence supports risks to the baby including reduced tone, poor feeding, jaundice, withdrawal, and sensorimotor impairment.8
Epidurals are a delivery method for narcotic pain-killers that pass through the placenta to the baby and have largely unpredictable effects on the birthing woman. Evidence supports risks to the baby including reduced tone, poor feeding, jaundice, withdrawal, and sensorimotor impairment.8
Physiologic risks to the mother include acute and persistent problems such as numbness, tingling, dizziness, respiratory paralysis, cardiac arrest, nerve injury, abscess, and death.910A user-friendly description of these considerations was explored by Pathways to Family Wellness, here.
Hurrying Up
When epidurals lengthen the second stage of labor, Pitocin, or synthetic mimic of the brain hormone, oxytocin, is delivered to augment the process. Because Pitocin does not cross the blood-brain barrier, it does not stimulate endorphin release. It also interferes with feedback loops suppressing natural oxytocin production while hyperstimulating the uterus without appropriate relaxation between contractions. The significance of this is just being revealed and may even reach to risk factors for autism.
Cutting Up
The increased risk of c-section1112 in the wake of epidural anesthesia is easily explained by relaxation of pelvic muscles that detach a woman from the instinctive guiding forces of an uninhibited labor, by the baby’s increased distress secondary to narcotic exposure and malposition, by the recruitment of Pitocin which causes uterine and therefore fetal distress, and fetal monitoring which, while superficially reassuring results in increased interventions (2-3x c-section rate) without improved outcomes.
Your doctor may fail to mention that a surgical birth brings with it these risk considerations: protracted recovery, infection (including necrotizing fasciitis), organ damage, adhesions, hemorrhage, embolism, hysterectomy, wound dehiscence, early infant separation, higher risk of respiratory problems for baby, and an exponentially increased risk of placenta accreta, a potentially lethal complication of surgical birth, contributing to a 3.6 fold increase in maternal death after cesarean relative to vaginal birth.
Of primary interest to clinicians who appreciate the role of the gut microbiome in child and adult health, abdicating a vaginal transfer of beneficial bacteria may set the stage for chronic disease including a 20% increased risk of obesity.
Opting out of epidural anesthesia: Choosing to feel
What are the best ways to help your body, mind, and spirit align for this tumultuous but life empowering journey?
Movement – Staying active during pregnancy is optimal mind-body medicine. Yoga, home-based routines, and swimming in unchlorinated water are excellent choices, at least 3 times weekly.
Chiropractic – With advanced perinatal training, holistic chiropractors are critical experts in proper alignment and nervous system support to facilitate a physiologic birth.
Acupuncture – Applied before and even during labor, acupuncture can gently and effectively facilitate a healthy labor and delivery. According to a Cochrane Review, acupuncture and hypnosis meet evidence-based efficacy criteria for pain management in labor.
Controlled Breathing/Meditation – Perhaps the most important tool for a new mother, learning to engage the relaxation response in pregnancy will help you to know what it feels like to be present to the labor experience, to go inward, quiet your mind, and release fear. Hypnobabies and hypnobirthing are well-regarded methodologies. If you are extremely anxious, breathing small amount of nitrous oxide mixed with oxygen can help.
Diet – The physical experience of labor and delivery is best supported by stocking the shelves up front for a healthy hormonal response with minimization of inflammation and maximization of nutrient-density. Eat sustainable, organic meat, fish, eggs, veggies including root vegetables and squash, fruit, nuts, and seeds. Leverage the complexity of food-based information to promote optimal gene expression in that growing baby, and support a healthy delivery and postpartum experience.
Doula – Preparation for labor, and support for mother and spouse have been traditionally left in the hands of a woman’s most doting partner, a doula. No woman should birth in a hospital without this advocate. Evidence supports a doula’s ability to help you achieve an intervention-free birth.
While my most heart-filling emails every day are from my homebirthing patients, I aim to sit in a place of true advocacy for the women that I treat and advise. I believe in informed consent, and I observe that this is not occurring in hospitals today. Explore resources that will help to expose you to the known risks and popularized benefits, so that you are making your own decision with your eyes wide open.
As most women who have experienced natural birth would attest – just when you think you can’t do it and your mind demands surrender – you meet your baby, and the world stands still in a moment of unparalleled beauty and wonder.
Sources:
1 http://www.ncbi.nlm.nih.gov/pubmed/15957994
2 http://www.ncbi.nlm.nih.gov/pubmed/12011872
3 http://www.ncbi.nlm.nih.gov/pubmed/24552992
4 http://www.ncbi.nlm.nih.gov/pubmed/12011872
6 http://www.nutricionhospitalaria.com/pdf/6395.pdf
7 http://www.internationalbreastfeedingjournal.com/content/1/1/24
8 http://www.ncbi.nlm.nih.gov/pubmed/12011872
9 http://onlinelibrary.wiley.com/doi/10.1016/S0091-2182%2897%2900052-9/abstract
10 http://www.ncbi.nlm.nih.gov/pubmed/17447690
12 http://summaries.cochrane.org/CD000331/epidurals-for-pain-relief-in-labour







One of the most compassionate experiences a woman can have is getting an epidural during childbirth. The realization that humanity is inherently good and that women don’t have to experience the worst pain of their lives in order to become mothers. The realization that you can push your baby out without pain.
Ladies, don’t let anyone tell you that you can’t push your babies out with an epidural or that you can’t love your babies if you have medical interventions in childbirth.
It’s not compassionate if you are harming yourself and your baby! It’s not the “worst pain of your life” by the way. Having a kidney stone is far worse! And, childbirth is more painful ultimately by HAVING an epidural since your chances of a C-section go sky high as a result. Recovering from a C-section is no picnic … having a baby naturally, you can go home within a few hours almost 100% pain-free! Looking at the experience holistically rather than clinically leads the THINKING woman to avoid epidurals as it TAKES AWAY HER POWER.
Something to add that I have not seen mentioned in any of the comments: some women (like myself) find the cervical checks during labor traumatic.
I was determined to get through labor without the epidural, but the dr shoving her hand inside me DURING a contraction immediately after she had agreed that she would not do that was traumatic, nd brought back flashbacks of past sexual abuse. I could not bear having to go through that again, and got an epidural before I would let her, or anyone, touch me again.
I really, really wish i had managed to go unmendicated though. I still feel like a complete failure, and have back pain, though i know the side effects could have been way worse. Now I’m pregnant again, and am planning on using a midwife. My first question to her was literally, you have other ways to check for progress besides internally, right?
From my three experiences I definitely agree that if you can and it is safe to so avoid any interference with the whole process. First two times I went into labour on my own and delivered with no particular drama. Pain wasn’t that bad and labour was quick. Third time round I had to be induced by various reasons that weren’t under my control. It was way more painful and unpleasant. I had to use epidural because it wasn’t impossible to bear. However, I have to say I was to relieved to be able to relax and baby came straight after with no problems and latched right away. My advice would be to go as natural as possible if it is safe to do so. But also trust your care providers and ask them to explain all your options in detail.
I can so relate to your post. I went into labor and have excruciating pain at 1c. It was horrific. I had done my research and knew I did not want pitocin, but the nurse kept coming back into the room and mentioning how I wasn’t progressing.. I kept saying no, maybe later. I feel like I was abused and treated like I didn’t have a voice. My doctor broke my water without asking.. even after I had a birth plan that mentioned not breaking the bag. I’m absolutely disgusted in hospitals and ob’s. I ended up with 2 epidural that stopped working – yes, you heard it right, stopped working. There’s too much to write on here.. at the end, I ended up in a c section.
If you have another baby, consider a birth center! MUCH BETTER CHOICE than a over-medicalized hospital birth! https://www.thehealthyhomeeconomist.com/21-reasons-to-have-your-baby-at-a-birthcenter/
Just really annoyed that you fail to mention inductions! Inductions, in my opinion are the main reason for increased c-sections. Forcing a body to labor that is not ready to labor! I went into labor at 40+5 days on my own. I asked for an epidural because my natural contractions were one on top of another and I was only 4cm. I never got a drop of pitocin during labor. I couldn’t catch my breath, I couldn’t regroup my thoughts. My doula tried everything but they wouldn’t ease up. I got the epidural and went from 4cm to complete in less than 15 min. My body was so tense that I couldn’t dilate and my baby was already at +2 station and I was beginning to have urges to push at 4 cm, which was dangerous! For me, it was a godsend.
Every woman needs to make informed medical decisions and they need to start by avoiding inductions.
Wow, lots of emotion and opinions from this article! Thank you to all the women who shared their experiences with and without an epidural. After supporting over 500 moms as a doula, I have seen many great births with and without an epidural. While I appreciate Dr Kelly’s information, I do think it could be more balanced and include the births where women are being induced, or just in so much pain, fear, exhaustion, that an epidural is the best path! The other pain medication options can be tried first. I have seen many babies latch right on and have no problem at all after an epidural and on the other hand I have seen babies struggle to get latch and mom need a lot of breastfeeding support with a totally natural birth. There are so many different paths to birthing and every mom needs to be respected and allowed to make the best decision for herself during her labor!