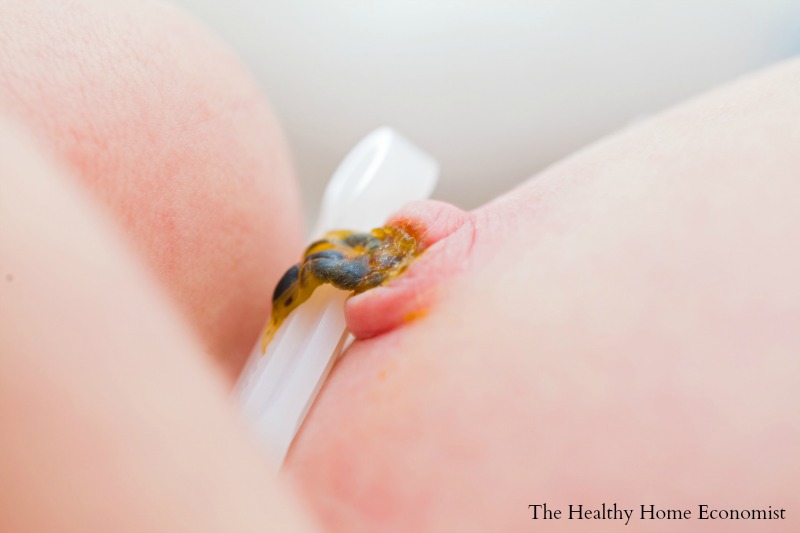
 Banking of a fetal stem cells after birth is an increasingly popular option for health savvy parents. It provides a sort of additional health insurance policy for baby and other family members. Fetal cord blood banking involves obtaining 3-5 oz of umbilical cord blood. Delayed cord clamping is not given as an option.
Banking of a fetal stem cells after birth is an increasingly popular option for health savvy parents. It provides a sort of additional health insurance policy for baby and other family members. Fetal cord blood banking involves obtaining 3-5 oz of umbilical cord blood. Delayed cord clamping is not given as an option.
Once retrieved, the blood is shipped to a cord blood bank where the stem cells are processed and preserved at sub zero temperature for a fee.
Benefits of Stem Cells from Cord Blood
To date, cord blood has been used to successfully treat over 70 diseases including leukemia, sickle cell anemia, non-Hodgkins lymphoma, and Hodgkins disease among others. Cord blood has a 25% chance of being a genetic match for full siblings and a 50% chance for parents. Of course, cord blood is a perfect match for the baby it came from.
Cord blood is preferred to bone marrow as it is less likely to cause life threatening rejection complications. As a result, using cord blood for a less than perfect match is more likely to work than a similar procedure using bone marrow. Cord blood is desirable, then, for extended family members as well. It has a much better chance than bone marrow of not being rejected. Cord blood is also a more pristine source for stem cells and is much less likely to be contaminated with viruses such as Epstein-Barr. Such pathogens can cause serious infections in transplant patients or those that are immunocompromised.
Rapid vs Delayed Cord Clamping
Many prospective parents do not realize that when they opt to bank their newborn baby’s cord blood, birth attendants are more likely to cut the umbilical cord early. This means within 30 seconds of birth! Rapid cord clamping ensures an adequate amount of cord blood is collected very easily.
This is not desirable for baby, however. The umbilical cord should never be cut until it has completely stopped pulsing. A study at the University of South Florida confirms that giving the baby all the cord blood improves outcome, even for healthy, full term infants.
Allowing all the cord blood to flow into the baby may take in excess of 3 full minutes. Cutting it prior to this point can deprive the baby of much needed oxygen. This is especially dangerous in those crucial minutes as the baby transitions to breathing on his/her own.
Health Issues from Early Clamping
Scientists have expressed concern that early clamping of the umbilical cord can lead to iron deficiency anemia, brain impairment, and even autism. David Hutchon, a consultant obstetrician at Darlington Memorial Hospital went so far as to call premature clamping of the umbilical cord “criminal” for at risk and vulnerable babies. This concern was borne out by a large scale study in 2007 of 1900 newborns where delayed cord cutting (2 minutes) reduced anemia by half and low iron levels by one third.
Problems from Delayed Clamping Unfounded
In babies where cord clamping is delayed, the chance of polycythemia and jaundice are heightened. This is due to an increased level of circulating red blood cells. However, this has proven to be of no concern in reality. In addition, the risk of excessive bleeding in the Mother does not appear to be significantly increased when there is a delay in cutting the umbilical cord.
In fact, delay in cord cutting appears to be of primary benefit to the baby and of little concern for the health of the mother. It may well prove inconvenient for hospital birthing staff, however. This is why discussion of your desire to delay the cord cutting needs to be discussed well in advance of the birth. Such a conversation is important even if you don’t plan to bank your baby’s cord blood!
Delayed Cord Clamping AND Fetal Stem Cells (yes, it’s possible!)
Do you wish to delay cord clamping and collect stem cells? Be sure to establish this goal with your OB or midwife right away. Clearly state your desire for the umbilical cord to be cut only once it stops pulsing. This signals that blood flow to your baby is maximized. Next, inform your practitioner about how to retrieve stem cells via alternative method.
How? The answer is from the placenta!
Once the placenta is delivered, the birthing staff can obtain plenty of cord blood to meet this need. It will likely take a bit more time and effort to retrieve the cord blood this way than from the umbilical cord. However, the extra effort is well worth it! There is no reason to avoid delayed cord clamping and potentially harm the newborn to obtain stem cells. Both goals are easily achieved if practitioners would simply think out of the box!
This is exactly the method I used, by the way. So, I know firsthand that it definitely works ♥.
Sarah, The Healthy Home Economist








6 percent of the shares in Mega Fon to Usmanov if Mega
Fon fails to do an IPO from the end of 2014, based on fair market
price my website the particular relation to its financing are often typed out by method
of a promissory notice or any other agreement.
I think it is great that you are writing about this. It is also possible to let the cord pulse for even ten minutes and still pull cord blood from the cord/placenta, according to a home birth midwife I know who has spoken with me about this recently. I am considering banking cord blood for my brother, who has leukemia at age 18 and may end up needing it to save his life. Despite all the issues with delayed cord cutting, I would gladly cut the cord early to save my brother’s life if I thought that were the only way. My baby will recover from less blood at birth, but my brother’s life may be saved by my baby’s unchosen gift. I’m a labor doula and childbirth educator planning a home birth, so I really do know how valuable the blood is to the newborn. I was much relieved when I learned A) I can do cord blood banking at a home birth and B) I can wait to collect the blood so the baby can get much of the blood herself. It’s definitely good to know.
Such a helpful post! Thank you so much!
When you see children who are alive today because of cord blood banking, it changes everything. This may not be too relevant, but you only get one chance to do this.
Oh, and for the 2nd birth where we let the cord pulse out completely and the placenta deliver before clamping, we dried and encapsulated the placenta for me to take post-partum — more info at http://placentabenefits.info/medicinal.asp. I suppose one could probably drain the cord blood, then still do this procedure.
Thank you for posting this article! In the hospital, although my birth plan asked for delayed cutting until the cord stopped pulsing, my 1st child's cord was cut immediately after she was born *because* she wasn't breathing right away. It makes no sense because this cut off her oxygen supply! Following this, my placenta didn't deliver, and it had to be manually removed. After my second birth, this time at home, my midwife let the cord pulse out completely and the placenta delivered before we cut the cord. Because of my placenta/cord issues and the research regarding anemia and blood volume to the baby, I've always felt the cord blood banking had some flaws — this article explained some of them. Thank you!
This would be a question for your midwife or OB. This procedure was done for my son's birth and the midwife told me that it takes extra work to do it this way, but that it can be done.
How do you get blood from the placenta and make sure it is not mom's blood mixed in?
Thank you for letting me know that there is an option to bank cord blood and still let the baby have all of their blood from the cord. My son was denied this blood because the doctor who performed our unplanned c-section didn't think it was important and ignored our wishes. Although we still aren't sure if we wish to bank cord blood it is good to know we have the option.
So glad to see this issue being addressed. Early cord clamping is a terrible injustice to the integrity of baby's immune system and overall constitution. Just another interventional assault causing compromises from day one on this side of the womb. Thanks so much for addressing the hard issues Sarah!
Teresa<><