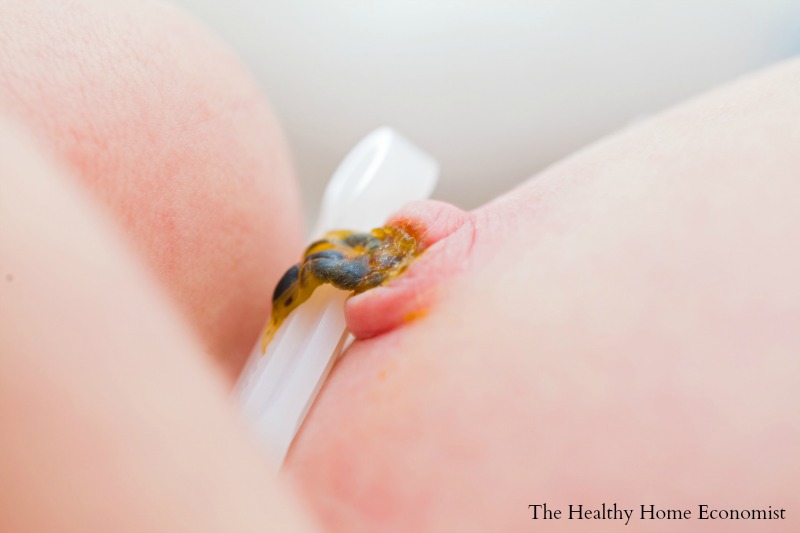
 Banking of a fetal stem cells after birth is an increasingly popular option for health savvy parents. It provides a sort of additional health insurance policy for baby and other family members. Fetal cord blood banking involves obtaining 3-5 oz of umbilical cord blood. Delayed cord clamping is not given as an option.
Banking of a fetal stem cells after birth is an increasingly popular option for health savvy parents. It provides a sort of additional health insurance policy for baby and other family members. Fetal cord blood banking involves obtaining 3-5 oz of umbilical cord blood. Delayed cord clamping is not given as an option.
Once retrieved, the blood is shipped to a cord blood bank where the stem cells are processed and preserved at sub zero temperature for a fee.
Benefits of Stem Cells from Cord Blood
To date, cord blood has been used to successfully treat over 70 diseases including leukemia, sickle cell anemia, non-Hodgkins lymphoma, and Hodgkins disease among others. Cord blood has a 25% chance of being a genetic match for full siblings and a 50% chance for parents. Of course, cord blood is a perfect match for the baby it came from.
Cord blood is preferred to bone marrow as it is less likely to cause life threatening rejection complications. As a result, using cord blood for a less than perfect match is more likely to work than a similar procedure using bone marrow. Cord blood is desirable, then, for extended family members as well. It has a much better chance than bone marrow of not being rejected. Cord blood is also a more pristine source for stem cells and is much less likely to be contaminated with viruses such as Epstein-Barr. Such pathogens can cause serious infections in transplant patients or those that are immunocompromised.
Rapid vs Delayed Cord Clamping
Many prospective parents do not realize that when they opt to bank their newborn baby’s cord blood, birth attendants are more likely to cut the umbilical cord early. This means within 30 seconds of birth! Rapid cord clamping ensures an adequate amount of cord blood is collected very easily.
This is not desirable for baby, however. The umbilical cord should never be cut until it has completely stopped pulsing. A study at the University of South Florida confirms that giving the baby all the cord blood improves outcome, even for healthy, full term infants.
Allowing all the cord blood to flow into the baby may take in excess of 3 full minutes. Cutting it prior to this point can deprive the baby of much needed oxygen. This is especially dangerous in those crucial minutes as the baby transitions to breathing on his/her own.
Health Issues from Early Clamping
Scientists have expressed concern that early clamping of the umbilical cord can lead to iron deficiency anemia, brain impairment, and even autism. David Hutchon, a consultant obstetrician at Darlington Memorial Hospital went so far as to call premature clamping of the umbilical cord “criminal” for at risk and vulnerable babies. This concern was borne out by a large scale study in 2007 of 1900 newborns where delayed cord cutting (2 minutes) reduced anemia by half and low iron levels by one third.
Problems from Delayed Clamping Unfounded
In babies where cord clamping is delayed, the chance of polycythemia and jaundice are heightened. This is due to an increased level of circulating red blood cells. However, this has proven to be of no concern in reality. In addition, the risk of excessive bleeding in the Mother does not appear to be significantly increased when there is a delay in cutting the umbilical cord.
In fact, delay in cord cutting appears to be of primary benefit to the baby and of little concern for the health of the mother. It may well prove inconvenient for hospital birthing staff, however. This is why discussion of your desire to delay the cord cutting needs to be discussed well in advance of the birth. Such a conversation is important even if you don’t plan to bank your baby’s cord blood!
Delayed Cord Clamping AND Fetal Stem Cells (yes, it’s possible!)
Do you wish to delay cord clamping and collect stem cells? Be sure to establish this goal with your OB or midwife right away. Clearly state your desire for the umbilical cord to be cut only once it stops pulsing. This signals that blood flow to your baby is maximized. Next, inform your practitioner about how to retrieve stem cells via alternative method.
How? The answer is from the placenta!
Once the placenta is delivered, the birthing staff can obtain plenty of cord blood to meet this need. It will likely take a bit more time and effort to retrieve the cord blood this way than from the umbilical cord. However, the extra effort is well worth it! There is no reason to avoid delayed cord clamping and potentially harm the newborn to obtain stem cells. Both goals are easily achieved if practitioners would simply think out of the box!
This is exactly the method I used, by the way. So, I know firsthand that it definitely works ♥.
Sarah, The Healthy Home Economist






I have been looking into cord blood banking, as I’m about to deliver my 2nd child in December. Many companies do now indicate that delayed cord clamping is an option and that an adequate sample may still be obtained when delayed cord clamping is practiced. Does anyone have experience with this or good results?
Thanks for finally talking about >Fetal Cord Blood Banking Discourages Delayed Cord Clamping?
The Healthy Home Economist <Loved it!
What a data of un-ambiguity and preserveness of valuable familiarity on the
topic of unpredicted emotions.
Professionally, if you ask me that will be better, iPhone or
Droid, I’d like the iPhone. It can help you find your misplaced iPhone easily.
It Is A novel approach to gaining feedback on just about anything.
Programs on the iPhone and Activities really are a popular feature for your iPhone.
At-least Siri always responds, perhaps requesting for clarification.
Each part presents the capabilities coresponding.
I am regular reader, how are you everybody? This paragraph posted at this site is genuinely nice.
Little Cook: This application created by Aqility ($3.ninety nine)
provides children a enjoyable introduction to cooking. Children discover to make their own choices as they combine ingredients in their own
virtual kitchen. They can make their preferred foods or zany creations
(onion and peanut butter sandwich, anyone?), and these
will then be examined by a professional kid-taster.
Children will improve their choice-making and culinary
skills, all while enjoying an engaging sport with colorful graphics.
The initial thing you want to do with your new iPad doesn’t actually happen on the iPad at all.
It occurs on your computer. If you don’t already have iTunes set up, you will want to download it and install it to your Pc.
Even if you have iTunes, you will want to make sure you are on the newest edition
by clicking on the Assist menu and selecting Check for Updates,
or if you use a Mac, select the iTunes menu and click on on Check for Updates.
You need to tap the Telephone icon and then tap the Keypad icon.
Once more tap and maintain the quantity one important and your Apple iphone
will start contacting the voicemail method.
You require to enter the current password, when prompted. Then
tap the quantity one key for Password Options,
adopted by choosing Set up or Change Passwords.
You need to enter the desired password in the password prompt,
and then tap # important. Press Finish to hang up your call.
Common things that have been reported are the incapability for the
home button to function, the phones, and microphones obtaining disabled,
unusual mistake messages when connecting your Iphone to your pc, and so on.
If you are going to use jailbreak then you should make sure that you have
a operating understanding of computers software and components.
These dismal numbers can mainly be blamed on the wait for the new Apple iPhone 5 keynote
announcement, which is rumored to be on Sept.
12th, 2012. On Sept. twenty first, the official Iphone 5 launch
date will allegedly take place. Through previous encounter, it may also be assumed that a 7 days prior to
the release, reservations ought to be possible via the online Apple Store.
The inside has an open up flooring strategy with a
gasoline fireplace, hardwoods flooring finished.
It also has a little bar and a scorching tub for residents to calming.
The exterior has a balcony and dormer windows. This home
located close to Sugarbush is one of the biggest
ski resorts in the East American – with an average of much
more than sixteen ft of snow falls right here annually.
Keep monitor of your diet plan in photographs.
Now everyone has listened to of keeping a food journal,
and everyone knows that this is an unrealistic factor to do in
apply. Nevertheless, a quick snap of your Iphone, and you have recorded what you are about
to eat. When you get a moment you can deliver the photographic information to GMail, exactly where you can tag every thing appropriately, then when
you are correlating your weight gains or losses with
what you have been consuming, all the necessary data will be effortlessly
at your finger tips.
On the other hand, the cost of the device seems to be over average for blood pressure cuffs of all sorts.
In addition, it isnt that easy to get the iPad on to the
dock, and you will most likely have to remove your
iPad from its situation. The wire that connects the cuff to the dock
is only 24 lengthy (about 70 cm) so your working area with the gadget is limited.
Finally, the iPad doesnt seem to match tightly sufficient into the dock.
I always spent my half an hour to read this web site’s posts every day along with a cup of coffee.
Very rapidly this site will be faous amid all blogging and
site-building people, due to it’s fastidious content